Overview
- Congress has not moved to extend enhanced ACA premium tax credits set to expire at the end of 2025, leaving subsidy levels scheduled to revert to lower pre-ARPA rates.
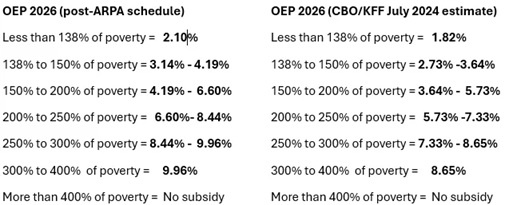
- The IRS’s newly published 2026 subsidy schedule raises the share of income households must pay for benchmark plans by more than a full percentage point at many income levels.
- CMS’s finalized Marketplace Integrity and Affordability Rule tightens income verification and inflation calculations while pausing enforcement of short-term plan duration limits.
- Preliminary insurer filings for 2026 propose a median premium increase of 18 percent, with many carriers seeking hikes above 20 percent and some states, such as Texas, averaging over 30 percent.
- Analysts warn that the combined impact of subsidy rollback, regulatory changes and medical inflation could drive net costs for subsidized enrollees up roughly 75 percent and shrink the marketplace risk pool.